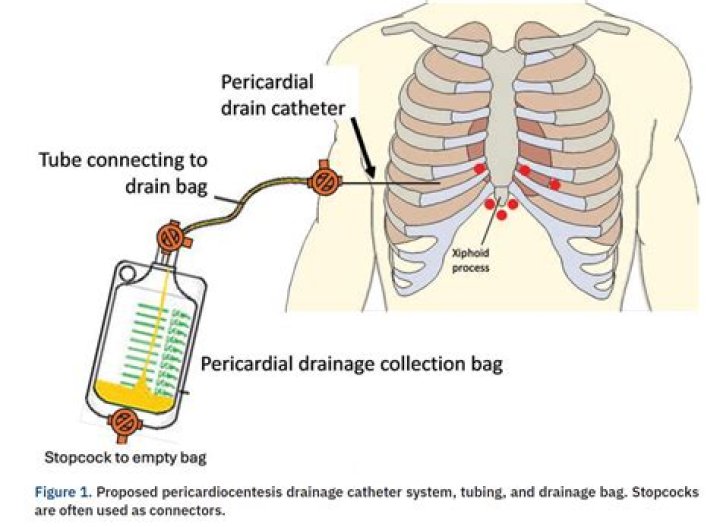
How to Flush Your Drainage Catheters - Turn the three-way stopcock off to the drainage bag.
- Clean the infusion port on the stopcock with an alcohol wipe and connect the flush syringe containing the appropriate amount of flush.
- Gently inject the flush into the drain towards the patient.
.
Subsequently, one may also ask, how do you remove a pericardial drain?
The pericardial catheter can be drained by gravity continuously or alternatively drained manually using sterile technique every 4 to 6 hours. Heparinized saline (2-3 cc) should be instilled into the catheter after each drainage attempt.
One may also ask, when should pericardial effusion be drained? Regardless if the pericardial effusion is transudative (consisting of watery fluid) or exudative (made up of protein-rich fluid), a large pericardial effusion causing respiratory symptoms or cardiac tamponade should be drained to remove the excess fluid, prevent its re-accumulation, or treat the underlying cause of the
Also know, how do they drain fluid from the heart?
Pericardiocentesis is a procedure done to remove fluid that has built up in the sac around the heart (pericardium). It's done using a needle and small catheter to drain excess fluid. A fibrous sac known as the pericardium surrounds the heart. Pericardiocentesis drains this fluid and prevents future fluid buildup.
What is a pericardial drain?
Pericardial drainage (pericardiocentesis) is done to find the cause of fluid buildup around the heart and to relieve pressure on the heart. The tissue sac that surrounds the heart is called the pericardium. It protects the heart and parts of the major blood vessels connected to the heart.
Related Question Answers
How long do chest tubes stay in after bypass surgery?
48 to 72 hours
Does fluid around the heart cause coughing?
Chronic coughing or wheezing - Fluid congestion (a buildup of fluid in the lungs) is common with heart failure, and is the reason why doctors often refer to it as "congestive heart failure" (CHF). This congestion can make you wheeze and cough. Some people cough up mucous or phlegm.What causes fluid buildup around the heart?
Pericardial effusion can result from inflammation of the pericardium (pericarditis) in response to illness or injury. Pericardial effusion can also occur when the flow of pericardial fluids is blocked or when blood accumulates within the pericardium, such as from a chest trauma.What are the symptoms of fluid around the heart?
Fluid around the heart symptoms - chest pain.
- a feeling of “fullness” in your chest.
- discomfort when you lie down.
- shortness of breath (dyspnea)
- difficulty breathing.
How do you get rid of fluid build up?
Water retention occurs when excess
fluids build up inside your body.
6 Simple Ways to Reduce Water Retention
- Eat Less Salt.
- Increase Your Magnesium Intake.
- Increase Vitamin B6 Intake.
- Eat More Potassium-Rich Foods.
- Try Taking Dandelion.
- Avoid Refined Carbs.
What is the most common cause of myocarditis?
According to the Myocarditis Foundation, viruses are one of the most common causes of infectious myocarditis. The most common viruses to cause myocarditis include Coxsackievirus group B (an enterovirus), Human Herpes Virus 6, and Parvovirus B19 (which causes fifth disease).How bad is fluid around the heart?
A pericardial effusion is excess fluid between the heart and the sac surrounding the heart, known as the pericardium. Most are not harmful, but they sometimes can make the heart work poorly. That fluid helps your heart move easier within the sac. If you have a pericardial effusion, much more fluid sits there.What are the 4 stages of heart failure?
There are 4 stages of heart failure (Stage A, B, C and D). The stages range from "high risk of developing heart failure" to "advanced heart failure," and provide treatment plans. Ask your healthcare provider what stage of heart failure you are in.What causes fluid in lungs and around heart?
Pulmonary edema is a condition caused by excess fluid in the lungs. In most cases, heart problems cause pulmonary edema. But fluid can accumulate for other reasons, including pneumonia, exposure to certain toxins and medications, trauma to the chest wall, and visiting or exercising at high elevations.What causes heart to enlarge?
An enlarged heart may be the result of a short-term stress on the body, such as pregnancy, or a medical condition, such as the weakening of the heart muscle, coronary artery disease, heart valve problems or abnormal heart rhythms. Treatment for an enlarged heart can include medications, medical procedures or surgery.What drugs cause pericardial effusion?
Causes of Pericardial Effusion Certain prescription drugs, such as hydralazine, a medication for high blood pressure; isoniazid, a tuberculosis drug; and phenytoin, a medication for epileptic seizures. Chemotherapy drugs, such as doxorubicin and cyclophosphamide.How long does it take to recover from pericardial effusion?
Recovery Time for Pericardial Effusion Treatment A patient treated with pericardial window will probably need to stay in the hospital for at least a few days, while a patient treated with pericardiectomy or pericardial stripping will probably be hospitalized for five to seven days.How long can you live with pericardial effusion?
Survival rates are consistently poor in patients with malignancy who present with a pericardial effusion. In our series, patients had a median survival of 2.6 months. Patients with lung cancer had a median survival of 2.1 months while those with other types of cancer of 4.7 months.Can pericardial effusion go away on its own?
If extra fluid builds up between the tissue layers, this is called pericardial effusion. Pericarditis is usually mild. It often goes away on its own or with rest and basic treatment. Severe cases need intensive treatment to prevent life-threatening complications.How common is pericardial effusion?
The study by Sagristà-Sauleda et al[11] included 322 patients, 132 with moderate and 190 with severe pericardial effusion. Cardiac tamponade was present in 37%. In this series, the most common diagnosis was acute idiopathic pericarditis which accounted for 20% of patients.How much pericardial fluid is normal?
Pericardial Effusion and Cardiac Tamponade The pericardial sac normally contains up to 50 mL of fluid; it can hold 80 to 200 mL of fluid acutely, and even up to 2 L if the fluid accumulates slowly.What is the difference between pericardial effusion and cardiac tamponade?
Pericardial effusion. Because of the limited amount of space in the pericardial cavity, fluid accumulation leads to an increased intrapericardial pressure which can negatively affect heart function. A pericardial effusion with enough pressure to adversely affect heart function is called cardiac tamponade.Can I work with pericarditis?
Current guidelines recommend that return to physical exercise or sport is permissible if there is no longer evidence of active disease. This includes the absence of fever, absence of pericardial effusion, and normalization of inflammatory markers (ESR and or C-reactive protein).What is Beck's triad?
Beck's triad is a collection of three medical signs associated with acute cardiac tamponade, an emergency condition wherein fluid accumulates around the heart and impairs its ability to pump blood. The signs are low arterial blood pressure, distended neck veins, and distant, muffled heart sounds.