What is normal chest tube drainage amount
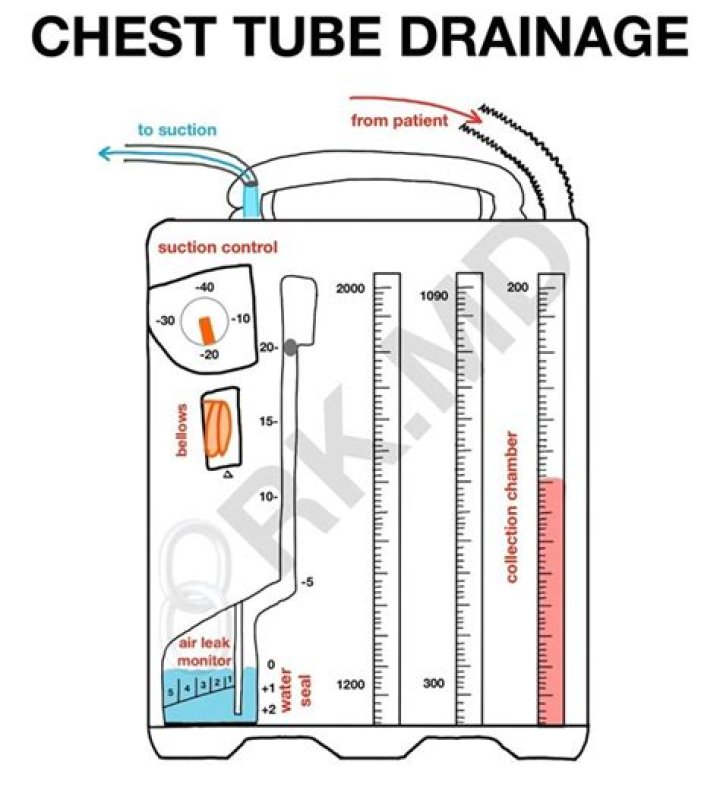
Compared to a daily volume drainage of 150 ml, removal of chest tube when there is 200 ml/day is safe and will even result in a shorter hospital stay.
What is normal chest tube output?
If the thoracostomy tube is placed for traumatic hemothorax, the indications for a thoracotomy include an initial sanguineous output of 1500 cc or an average of 200 cc/hr over 4 hours consecutive hours.
How do you measure a chest tube?
Measure the length between the skin incision and the apex of the lung to estimate how far the chest tube should be inserted. If desired, place a clamp over the tube to mark the estimated length. Some prefer to clamp the tube at a distal point, memorizing the estimated length.
How much should a chest tube drain per hour?
7.1 Place container upright on floor. 7.2 Mark and date drainage, at eye level, on collection chamber. 7.3 Record. Pediatric: 3 mL/Kg/hour in a 3 hour period or 5 to 10 mL/Kg in any 1 hour period.How much fluid does a JP drain hold?
The drain(s) is left in place until drainage is approximately 30 cc’s or less (or 30 ml’s, or 1 ounce) per drain for each of 2 consecutive days. The fluid which collects in the bulb is normally very red at first, changing to more orange or straw-colored the longer it is in place.
Is continuous bubbling normal in chest tube?
Air bubbling through the water seal chamber intermittently is normal when the patient coughs or exhales, but if there is continuous air bubbling in the chamber, it can indicate a leak that should be evaluated.
How much drainage is normal after open heart surgery?
Drainage volumes plateau to 31 mL per hour, 8 hours after surgery. From 24 to 48 hours, the mean drainage was 21 mL per hour. Drainage volumes varied between genders.
Does the size of chest tube matter?
Conclusions: For injured patients with chest trauma, chest tube size did not impact the clinically relevant outcomes tested. There was no difference in the efficacy of drainage, rate of complications including retained hemothorax, need for additional tube drainage, or invasive procedures.Should a chest drain bubble?
Air Leak (bubbling) Continuous bubbling of this chamber indicates large air leak between the drain and the patient. Check drain for disconnection, dislodgement and loose connection, and assess patient condition. Notify medical staff immediately if problem cannot be remedied.
What size Hemothorax needs a chest tube?Both American and Japanese trauma care guidelines recommend large-bore (36–40 Fr in the ATLS and 28 Fr in the JATEC) chest tubes.
Article first time published onHow many chest tubes are placed per year?
Clinicians place chest tubes approximately 1 million times each year in the United States, but little information is available to guide their management. Specifically, use of the rate of pleural fluid drainage as a criterion for tube removal is not standardized.
How much drainage is normal after surgery?
The amount of serosanguineous fluid should decrease each day and the color of the fluid will turn light pink or light yellow. Your surgeon will usually remove the bulb when drainage is below 25 ml per day for two days in a row. On average, JP drains can continue to drain for 1 to 5 weeks.
How much comes out of JP drain?
The Jackson-Pratt drain is usually removed when the drainage is 30 mL or less over 24 hours. You’ll write down the amount of drainage you have in the drainage log at the end of this resource.
What color should JP drain be?
Pay attention to fluid color and measurements Drainage is bloody following surgery, but as time passes it should become straw-colored, then clear. Discharge should never look cloudy or like pus. If it does, contact your physician. The amount of fluid will decrease as time passes.
How much chest tube drainage is normal after CABG?
Depending on the nature of the surgery, there may be as many as four chest tubes in place, but two to three is typical. The tubes are typically removed within 48 to 72 hours after open heart surgery unless there is more drainage than is typical, or the surgeon determines that there is a reason for the tubes to stay.
What color should drainage be after surgery?
When you first get the drain, the fluid will be bloody. It will change colour from red to pink to a light yellow or clear as the wound heals and the fluid starts to go away. Your doctor may give you information on when you no longer need the drain and when it will be removed.
Why is chest tube drainage important after cardiac surgery?
Introduction. Drainage of fluid, or evacuation of air, from the pericardial and pleural spaces after cardiothoracic surgery is necessary to prevent effusions, tamponade or pneumothoraces and to also detect hemorrhage. Therefore negative pressure drains are placed in the mediastinum and pleural cavities.
What does an air leak look like in a chest tube?
Start by examining the air-leak detection chamber in the water seal of the drainage device. An air leak presents as small air bubbles; the amount of bubbling indicates the degree of the leak. If you notice bubbling, determine location of the leak.
How do you know if there is an air leak in a chest tube?
Once a chest tube is inserted, air bubbling into the chest drainage system indicates an air leak. The flow of air through the fistulous tract into the pleural space delays healing and inhibits lung expansion.
How do you know a chest tube is working properly?
The water in the water-seal chamber should rise with inhalation and fall with exhalation (this is called tidaling), which demonstrates that the chest tube is patent. Continuous bubbling may indicate an air leak, and newer systems have a measurement system for leaks — the higher the number, the greater the air leak.
How do you assess a chest drain?
- Location: …
- Pain.
- Swing/Oscillation – Normal – reflects the changes in pleural pressure on breathing (if not on suction). …
- Draining- Denotes volume of fluid draining from pleural space. …
- Bubbling- Reflects the amount of air draining out of the pleural space.
How much fluid can be removed from lungs?
For therapeutic purposes, removing 400-500 mL of the pleural fluid is often sufficient to reduce shortness of breath. The usual recommended limit is 1000-1500 mL in a single thoracentesis procedure.
What does it mean if a chest drain is not swinging?
Therefore, if a chest drain is not swinging, it is not in connection with the pleural space either through blockage, kinking or withdrawal to the thoracic wall. Bubbling – In a pneumothorax, air leaks into the pleural space.
What size of chest tube would you use in the management of trauma related pneumothorax?
Generally, large- bore chest tubes (32–40 Fr) are used for the treatment of traumatic pneumothorax and hemothorax. Traditionally, a tube with a large diameter has been the standard, as both air and blood are thought to be better removed from the pleural cavity with the large tube.
What is water seal chest tube?
The middle chamber of a traditional chest drainage system is the water seal. The main purpose of the water seal is to allow air to exit from the pleural space on exhalation and prevent air from entering the pleural cavity or mediastinum on inhalation.
Why is a triangle safe?
It is the preferred site for chest tube insertion, as it minimizes the risk of injury to internal organs, vascular structures such as the internal mammary artery, muscles and breast tissue [2]. However, complications associated with insertion of chest tube drainage in the ‘safe triangle’ are also known.
Is a pigtail catheter the same as a chest tube?
Small-bore chest tubes – also referred to as pigtail catheters – are being used to relieve both spontaneous and in some cases, traumatic pneumothorax. These pigtails are placed with a Seldinger catheter-over-wire technique very similar to the central venous catheter insertion.
When do you use a Hemothorax chest tube?
A chest tube is usually put to water seal after the lung is fully reexpanded on radiography, fluid drainage is less than 50 mL in 24 hours, and no significant residual air leak is present.
What is the difference between thoracotomy and Thoracostomy?
Thoracotomy is surgery that makes an incision to access the chest. It’s often done to remove part or all of a lung in people with lung cancer. Thoracostomy is a procedure that places a tube in the space between your lungs and chest wall (pleural space).
What is considered high chest tube output?
High-output chest tube drainage was defined as drainage greater than 250 mL per 24 hour period.
How much pleural fluid can be drained in a day?
Pleural fluid drainage should to be started immediately and up to 1500 mL of fluid can be removed. After removing the pleural fluid, a chest radiograph or postprocedural CT scan should be obtained to confirm the appropriate position of the pigtail catheter and evaluate possible complications including pneumothorax.

