What does denial Code N362 mean?
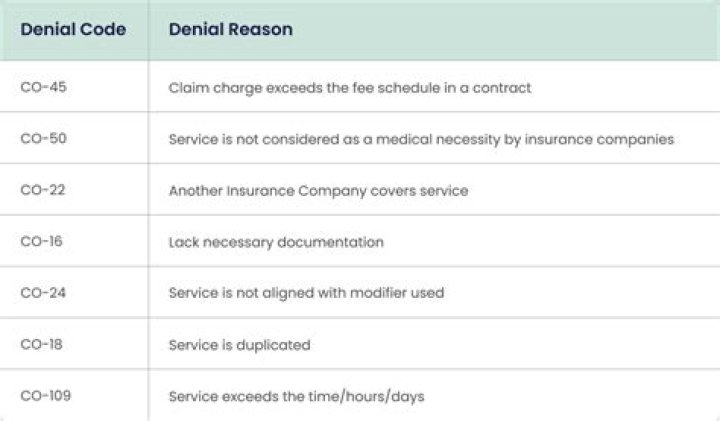

What does denial Code N362 mean?
prior processing information incorrect
CO/119/N362. Payment denied – prior. processing information. incorrect.
What is denial code PR 177?
PR 177 Payment denied because the patient has not met the required eligibility requirements.
What is PR denial code?
What does the denial code PR mean? PR Meaning: Patient Responsibility (patient is financially liable). A provider is prohibited from billing a Medicare beneficiary for any adjustment amount identified with a CO group code, but may bill a beneficiary for an adjustment amount identified with a PR group code.
What is denial code M77?
Remark Code: M77. Missing/incomplete/invalid place of service.
What is the purpose of medical claims clearinghouse?
The Clearing House or TPA picks up claims from your hospital’s billing software, gathers and processes documentation for each patient, and passes them on to the insurance provider. They coordinate with dozens of insurance service providers, for each patient who passes through your hospital.
What does indemnification adjustment Medicare?
Medicare indemnifies the beneficiary (and recovers from the provider, practitioner, or supplier), if the following conditions are met: 1 The amount of indemnification is the total that the beneficiary paid the provider, practitioner, or supplier.
What does denial code B11 mean?
claim/service has been transferred to
B11 The claim/service has been transferred to the proper payer/processor for processing. Claim/service not covered by this payer/processor.
What is denial code N95?
RA Remark Code N95 – This provider type/provider specialty may not bill this service. MSN 26.4 – This service is not covered when performed by this provider.
What is remark code n4?
CO 4 Denial Code: The procedure code is inconsistent with the modifier used or a required modifier is missing. You are receiving this reason code when a claim is submitted and the procedure code(s) are billed with the wrong modifier(s), or the required modifier(s) are missing.