What does APD mean in ophthalmology
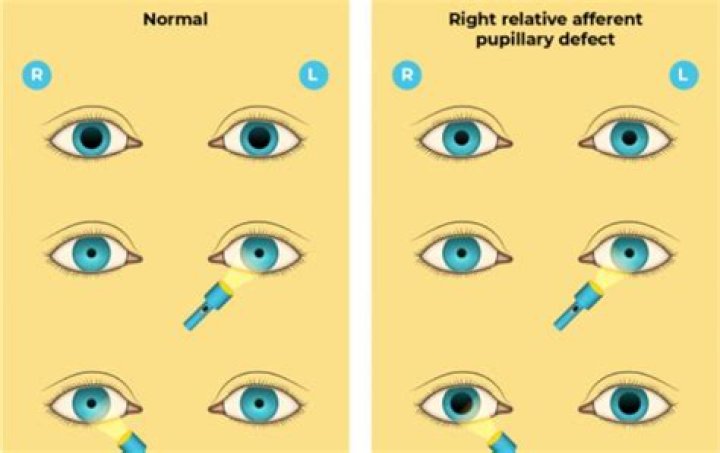
An Afferent Pupillary Defect
Can you have an APD in both eyes?
In case if both pupils do not show a similar response to the light stimuli, shone in one eye at a time, the patient will be diagnosed with RAPD or Marcus Gunn pupils. off note if the condition is bilateral and symmetrical, there will not be a RAPD but bilateral APD.
What is the difference between APD and RAPD?
RAPD vs APD In literature, and clinical practice, RAPD, and APD, or afferent pupillary defect, may be used synonymously. However, RAPD is technically describing the relative response of one pupil so there is no such thing as bilateral RAPD and, for a RAPD to exist, the damage must be asymmetric between the eyes.
What causes an afferent pupillary defect?
Common causes of unilateral optic nerve disorders that can be associated with a RAPD include ischaemic optic neuropathy, optic neuritis, optic nerve compression (orbital tumours or dysthyroid eye disease), trauma, and asymmetric glaucoma.What is efferent pupillary defect?
Efferent pupillary defects are caused by problems of sympathetic or parasympathetic innervation or structural iris changes presenting as anisocoria or impaired pupillary light reaction. This overview describes the diagnostic steps for evaluating efferent pupillary disorders and outlines further steps of work-up.
Can optic neuritis be detected in an eye exam?
An eye doctor, either an ophthalmologist or optometrist, can diagnose optic neuritis. They can perform tests to check color vision, how eyes respond to light, and how well the eye can see detail, such as letters in an eye chart.
How is APD measured in ophthalmology?
Most commonly, the presence of an APD is evaluated in office using the swinging flashlight test, in which each pupil is illuminated and the velocity and amplitude of the pupillary response is compared. In a healthy patient, light stimulation into one pupil results in equal constriction of both.
What is the Argyll Robertson pupil?
The Argyll Robertson (AR) pupil has been defined as a pupil that is small and constricts poorly to direct light but briskly when a target within reading distance is viewed (“light-near dissociation”).Why do pupils dilate in Rapd?
The pathologic response that characterizes the RAPD includes the following: 1) the light reaction causes pupil constriction in both eyes when the light shines in the normal eye, and (2) dilatation of the pupils in both eyes when the light stimulus is rapidly transferred from the normal eye to the pathologic eye.
What lesion causes Rapd?The most common cause of Marcus Gunn pupil is a lesion of the optic nerve (between the retina and the optic chiasm) due to glaucoma, or severe retinal disease, or due to multiple sclerosis. It is named after Scottish ophthalmologist Robert Marcus Gunn.
Article first time published onWhat is ischemia of the eye?
Ischemic optic neuropathy (ION) is when blood does not flow properly to your eye’s optic nerve, eventually causing lasting damage to this nerve. With ION, you suddenly lose your vision in one or both of your eyes.
Does amblyopia cause APD?
Pathology responsible for causing an APD can include significant amblyopia, major retinal issues and optic neuropathy.
What is optic nerve neuritis?
Optic neuritis is a condition that affects the eye and your vision. It occurs when your optic nerve is inflamed. The optic nerve sends messages from your eyes to your brain so that you can interpret visual images.
Why is there Rapd in CRVO?
The ischemic type is in sharp contrast to the nonischemic because there is significant retinal capillary obliteration in ischemic CRVO. 3. The relative afferent pupillary defect (RAPD) is very helpful in separating the ischemic type from the nonischemic type, during both the early and the late stages of the disease.
What is a Marcus Gunn pupil?
Marcus Gunn pupil (MGP) is the term given to an abnormal pupil showing aberrant pupillary response in certain ocular disorders. In literature, the term is often used synonymously with Marcus Gunn phenomenon or relative afferent pupillary defect (RAPD). [1] After exposure to bright light, a normal pupil constricts.
Which part of the brain controls pupillary changes?
The hypothalamus is the control center for many homeostatic mechanisms. It regulates both autonomic function and endocrine function. The roles it plays in the pupillary reflexes demonstrates the importance of this control center.
How do I check my ophthalmology motility?
When testing motility, assess the eye alignment in primary gaze (consider using the Hirschberg test) and then have the patient move the eyes in an “H” pattern, as shown in Figure 1. Using your finger, a light or a toy, trace an “H” pattern in front of the patient while instructing them to hold their head still.
What does a Pachymeter do?
Pachymetry – A Simple Test to Determine Corneal Thickness A pachymetry test is a simple, quick, painless test to measure the thickness of your cornea. With this measurement, your doctor can better understand your IOP reading, and develop a treatment plan that is right for your condition.
What is the medical term for both eyes?
OU refers to Oculus Uterque. It stands for both eyes. These are the traditional abbreviations that doctors use when making prescriptions for eyeglasses.
What is the most common cause of optic neuritis?
The most common cause for ON is inflammatory demyelination of the optic nerve. Demyelination is a process in which the myelin is stripped off by disease. It is believed that ON is an autoimmune process, where for some unknown reason the immune system attacks tissues of the body causing injury.
Can optic neuritis be caused by stress?
In fact, continuous stress and elevated cortisol levels negatively impact the eye and brain due to autonomous nervous system (sympathetic) imbalance and vascular dysregulation; hence stress may also be one of the major causes of visual system diseases such as glaucoma and optic neuropathy.
What does vision look like with optic neuritis?
An episode of Optic Neuritis typically begins with eye pain, especially with eye movements. Within a few days, patients will notice blurred vision in the affected eye. Often this appears like a “thumb-print” or smudge that blurs the vision. Within a week, this may progress to darkening of part of the visual field.
What is optic atrophy?
Optic atrophy type 1 is a condition that often causes slowly worsening vision, usually beginning in childhood. People with optic atrophy type 1 typically experience a narrowing of their field of vision (tunnel vision). Affected individuals gradually lose their sight as their field of vision becomes smaller.
Why does Argyll Robertson pupil happen?
Argyll Robertson pupil is found in late-stage syphilis, a disease caused by the spirochete Treponema pallidum. Neurosyphilis occurs due to an invasion of the cerebrospinal fluid (CSF) by the spirochete which likely occurs soon after the initial acquisition of the disease.
Why is Argyll Robertson pupil constricted?
The Argyll Robertson pupil occurs when a disease interferes with the light reflex pathway, thereby inhibiting the pupil’s natural response to bright light. Specifically, Argyll Robertson pupils don’t constrict in response to light but do constrict to focus on a nearby object.
Why does light near dissociation occur?
Description. Light-near dissociation (LND) is a pupillary sign that occurs when the pupillary light reaction is impaired while the near reaction (accommodative response) remains intact.
How do you test a swinging flashlight?
To perform this test, shine a penlight into one eye to attain maximum pupil constriction, then quickly switch the light source to the other eye and back again. Normally, the second eye should respond with the same pupillary constriction as the first eye as a result of a consensual response.
Does glaucoma cause Rapd?
RAPD can be observed in cases of asymmetrical retinal or optic nerve damage, including glaucomatous optic neuropathy. Although primary open-angle glaucoma usually affects both eyes, it is often an asymmetric disease.
Is NAION an eye stroke?
Non-arteritic anterior ischemic optic neuropathy (NAION) is a potentially debilitating condition that occurs from a lack of sufficient blood flow to the optic nerve. If you have sudden vision loss, contact your doctor immediately.
Can vision return after eye stroke?
You may regain your vision after an eye stroke. Most people are left with some vision loss. Some cases can lead to blindness.
Can an eye stroke lead to a brain stroke?
Keep in mind that the blood circulation to the retina is the same circulation that flows to the front of the brain, so eye strokes and brain strokes are connected in that way. Also, eye strokes are a significant risk factor for experiencing a brain stroke.