What causes dehiscence in wounds
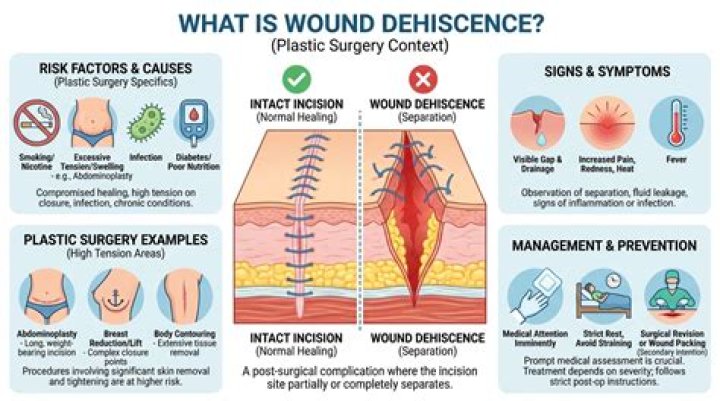
The causes of dehiscence are similar to the causes of poor wound healing and include ischemia, infection, increased abdominal pressure, diabetes, malnutrition, smoking, and obesity. [1] Superficial dehiscence is when the wound edges begin to separate and by increased bleeding or drainage at the site.
What can you do for wound dehiscence?
If an abdominal wound dehiscence is not treated, it can lead to wound evisceration — a medical emergency in which internal organs stick out through the incision. Treatment for wound dehiscence can involve medicines to fight pain and treat infection, and surgery to remove dead tissue and repair the wound.
How can dehiscence be prevented?
- maintaining blood volume through adequate fluid replacement.
- maintaining warmth (to prevent vasoconstriction)
- aggressively managing pain (to prevent vasoconstriction)
- using supplemental oxygen when needed to maintain normal oxygen levels.
What increases risk of dehiscence?
What Are Risk Factors for Dehiscence? A variety of underlying health conditions can increase a patient’s risk for developing dehiscence after surgery. Such conditions include the patient being overweight or obese, hypertension, anemia, and hypoproteinemia.Is wound dehiscence normal?
Wound dehiscence is a distressing but common occurrence among patients who have received sutures. The condition involves the wound opening up either partially or completely along the sutures – basically, the wound reopens to create a new wound.
Why is there a hole in my incision?
A clean wound will have minimal space between the edges of the wound and will commonly form a straight line. If your stitches, staples, or surgical glue have split apart, or if you see any holes forming in the wound, you’re experiencing dehiscence.
How common is wound dehiscence?
Wound dehiscence is estimated to occur in 0.5–3.4% of abdominopelvic surgeries, and carries a mortality of up to 40%.
Is wound dehiscence an emergency?
Complications of Wound Dehiscence Complete wound dehiscence is a medical emergency, as it can lead to evisceration, where internal organs protrude through the wound.What helps a deep wound heal faster?
- Antibacterial ointment. A person can treat a wound with several over-the-counter (OTC) antibacterial ointments, which can help prevent infections. …
- Aloe vera. …
- Honey. …
- Turmeric paste. …
- Garlic. …
- Coconut oil.
Complications of Removing Stitches Wound reopening: If sutures are removed too early, or if excessive force is applied to the wound area, the wound can reopen. The doctor may restitch the wound or allow the wound to close by itself naturally to lessen the chances of infection.
Article first time published onWhy is my wound not closing?
A skin wound that doesn’t heal, heals slowly or heals but tends to recur is known as a chronic wound. Some of the many causes of chronic (ongoing) skin wounds can include trauma, burns, skin cancers, infection or underlying medical conditions such as diabetes. Wounds that take a long time to heal need special care.
How does infection cause dehiscence?
The causes of dehiscence are similar to the causes of poor wound healing and include ischemia, infection, increased abdominal pressure, diabetes, malnutrition, smoking, and obesity. [1] Superficial dehiscence is when the wound edges begin to separate and by increased bleeding or drainage at the site.
What are two common causes of postoperative wound evisceration Why might these causes lead to wound evisceration?
There are four main causes: suture tearing through the fascia, knot failure, suture failure, and extrusion of abdominal contents between sutures placed too far apart. At least 50% of the cases are due to technical error with a potentially lethal result.
What is the clear fluid that comes out of a wound?
If the drainage is thin and clear, it’s serum, also known as serous fluid. This is typical when the wound is healing, but the inflammation around the injury is still high. A small amount of serous drainage is normal. Excessive serous fluid could be a sign of too much unhealthy bacteria on the surface of the wound.
Which patient group would be at increased risk of wound dehiscence?
Patients older than 65 years are more likely to develop wound dehiscence because of deterioration in tissue repair mechanism compared with younger patients [3]. Other well-known risk factors include hypoproteinemia, local wound infection, anemia, hypertension, and emergency surgery [1].
How do you know if you have wound dehiscence?
You may notice the following when your wound starts to come apart: A feeling that the wound is ripping apart or giving way. Leaking pink or yellow fluid from the wound. Signs of infection at the wound site, such as yellow or green pus, swelling, redness, or warmth.
Is my wound infected or just healing?
Discharge. After the initial discharge of a bit of pus and blood, your wound should be clear. If the discharge continues through the wound healing process and begins to smell bad or have discoloration, it’s probably a sign of infection.
What prevents wounds from healing?
Wound healing can be delayed by factors local to the wound itself, including desiccation, infection or abnormal bacterial presence, maceration, necrosis, pressure, trauma, and edema. Desiccation.
What is dehiscence how is it different from evisceration?
Dehiscence is secondary to technical failure of sutures, shear forces from tension, or fascial necrosis from infection and/or ischemia (2). Evisceration is the uncontrolled exteriorization of intraabdominal contents through the dehisced surgical wound outside of the abdominal cavity.
What happens when your incision opens up?
If you incision breaks open, call your doctor. Your doctor may decide not to close it again with stitches. If that happens, your doctor will show you how to care for your incision a different way. This will likely involve the use of bandages to absorb the drainage that comes from the incision.
Why is my operation wound not healing?
A non-healing surgical wound can occur after surgery when a wound caused by an incision doesn’t heal as expected. This is usually caused by infection – a rare but serious complication. Causes of poor wound-healing depend on the type and location of the procedure, health condition and other factors.
Does salt water heal wounds?
The healing powers of saltwater are primarily a myth. Especially when a wound is just beginning to heal, it is advisable to protect the wound from direct contact with tap water. Water and moisture cause the skin to swell and this can impair wound healing.
What vitamins help with wound healing?
Vitamins and minerals Vitamin A, vitamin C and zinc help your body to repair tissue damage, fight infections, and keep your skin healthy.
What does white skin around a wound mean?
Maceration occurs when skin has been exposed to moisture for too long. A telltale sign of maceration is skin that looks soggy, feels soft, or appears whiter than usual. There may be a white ring around the wound in wounds that are too moist or have exposure to too much drainage.
Which abdominal incision is most likely to be a factor in the cause of dehiscence?
Transverse incisions are generally considered to dehiscence much less than the vertical incision. The suture should have excellent handling and knotting.
When is it too late to cut wounds?
Your risk of infection increases the longer the wound remains open. Most wounds that require closure should be stitched, stapled, or closed with skin adhesives (also called liquid stitches) within 6 to 8 hours after the injury. Some wounds that require treatment can be closed as long as 24 hours after the injury.
When is a wound debridement needed?
Debridement isn’t required for all wounds. Typically, it’s used for old wounds that aren’t healing properly. It’s also used for chronic wounds that are infected and getting worse. Debridement is also necessary if you’re at risk for developing problems from wound infections.
What deficiency causes slow healing?
Vitamin C has many roles in wound healing, and a deficiency in this vitamin has multiple effects on tissue repair. Vitamin C deficiencies result in impaired healing, and have been linked to decreased collagen synthesis and fibroblast proliferation, decreased angiogenesis, and increased capillary fragility.
Should you let air get to a wound?
A: Airing out most wounds isn’t beneficial because wounds need moisture to heal. Leaving a wound uncovered may dry out new surface cells, which can increase pain or slow the healing process.
Which ointment is best for wound?
A first aid antibiotic ointment (Bacitracin, Neosporin, Polysporin) can be applied to help prevent infection and keep the wound moist. Continued care of the wound is also important. Three times a day, wash the area gently with soap and water, apply an antibiotic ointment, and re-cover with a bandage.
How do you dry a weeping wound?
Don’t get your wound wet in the bath or shower. You can keep your wound dry by using a cast/wound protector or using Press-N-Seal plastic wrap to cover the wound area then tape a kitchen trash bag over the wound/dressing. If your wound can’t be protected, a sponge bath is recommended.

