What are the compensatory mechanisms of heart failure?
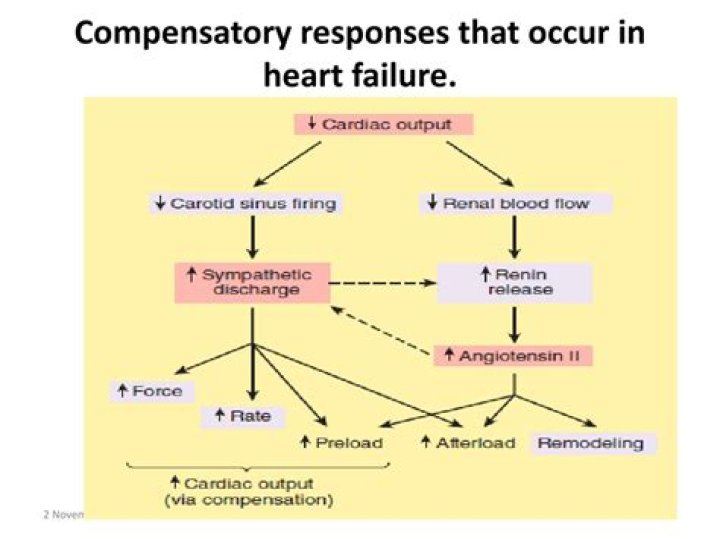
.
Keeping this in consideration, which of the following is a compensatory mechanism for decreased cardiac output in heart failure?
Cardiac dysfunction precipitates changes in vascular function, blood volume, and neurohumoral status. These changes serve as compensatory mechanisms to help maintain cardiac output (primarily by the Frank-Starling mechanism) and arterial blood pressure (by systemic vasoconstriction).
Also Know, what are the 4 stages of congestive heart failure? There are 4 stages of heart failure (Stage A, B, C and D). The stages range from "high risk of developing heart failure" to "advanced heart failure," and provide treatment plans. Ask your healthcare provider what stage of heart failure you are in.
In this manner, what is the pathophysiology of heart failure?
The main pathophysiology of heart failure is a reduction in the efficiency of the heart muscle, through damage or overloading. A reduced stroke volume may occur as a result of a failure of systole, diastole or both. Increased end systolic volume is usually caused by reduced contractility.
What body systems are affected by congestive heart failure?
As a result, the kidneys may respond by causing the body to retain fluid (water) and salt. If fluid builds up in the arms, legs, ankles, feet, lungs, or other organs, the body becomes congested, and congestive heart failure is the term used to describe the condition.
Related Question AnswersWhat affects cardiac output?
Factors affect cardiac output by changing heart rate and stroke volume. Primary factors include blood volume reflexes, autonomic innervation, and hormones. Secondary factors include extracellular fluid ion concentration, body temperature, emotions, sex, and age.What is the normal cardiac output?
Medical Definition of Cardiac output The amount of blood put out by the left ventricle of the heart in one contraction is called the stroke volume. The stroke volume and the heart rate determine the cardiac output. A normal adult has a cardiac output of 4.7 liters (5 quarts) of blood per minute.What is meant by heart failure?
Heart failure is a condition in which the heart can't pump enough blood to meet the body's needs. In some cases, the heart can't fill with enough blood. In other cases, the heart can't pump blood to the rest of the body with enough force. However, heart failure is a serious condition that requires medical care.What causes decreased cardiac output?
A bradycardia may be the primary cause of low cardiac output. Hypothyroidism, hypothermia, drugs such as beta blockers and calcium channels blockers, inferior myocardial ischemia and conduction system dysfunction may all cause significant bradycardia.What can worsen heart failure?
Medications that may increase the risk of heart problems include nonsteroidal anti-inflammatory drugs (NSAIDs); certain anesthesia medications; some anti-arrhythmic medications; certain medications used to treat high blood pressure, cancer, blood conditions, neurological conditions, psychiatric conditions, lungWhat is the role of RAAS in heart failure?
In heart failure with a low cardiac output state, activation of the RAAS serves as a compensatory mechanism to maintain cardiac output. Reduced renal blood flow and sodium delivery to the distal tubule leads to renin release, which is exacerbated further by increased sympathetic tone.How do you measure cardiac output?
Cardiac output is the volume of blood the heart pumps per minute. Cardiac output is calculated by multiplying the stroke volume by the heart rate. Stroke volume is determined by preload, contractility, and afterload.What is Neurohumoral response?
Neurohumoral activation refers to increased activity of the sympathetic nervous system, renin-angiotensin system, vasopressin and atrial natriuretic peptide.What is the pathophysiology of a disease?
Pathophysiology is the study of the changes of normal mechanical, physical, and biochemical functions, either caused by a disease or resulting from an abnormal syndrome. From: Haematology Case Studies with Blood Cell Morphology and Pathophysiology, 2017.How do you classify heart failure?
NYHA Classification - The Stages of Heart Failure:- Class I - No symptoms and no limitation in ordinary physical activity, e.g. shortness of breath when walking, climbing stairs etc.
- Class II - Mild symptoms (mild shortness of breath and/or angina) and slight limitation during ordinary activity.
How do you evaluate heart failure?
Advertisement- Blood tests. Your doctor may take a blood sample to look for signs of diseases that can affect the heart.
- Chest X-ray.
- Electrocardiogram (ECG).
- Echocardiogram.
- Stress test.
- Cardiac computerized tomography (CT) scan.
- Magnetic resonance imaging (MRI).
- Coronary angiogram.
How does heart failure cause tachycardia?
Tachycardia occurs when an abnormality in the heart produces rapid electrical signals that quicken the heart rate, which is normally about 60 to 100 beats a minute at rest. But if left untreated, tachycardia can disrupt normal heart function and lead to serious complications, including: Heart failure.What is the most common cause of right heart failure?
Some other causes of right-side heart failure include: Coronary artery disease . This is the most common form of heart disease and cause of heart failure. When you have coronary artery disease, plaque blocks your arteries, causing blood flow to your heart muscle to slow or even stop.What is the difference between systolic heart failure and congestive heart failure?
Systolic heart failure occurs when the left ventricle fails to contract normally. This reduces the level of force available to push blood into circulation. Without this force, the heart can't pump properly. Diastolic failure, or diastolic dysfunction, happens when the muscle in the left ventricle becomes stiff.What is the anatomy and physiology of the heart?
The heart is a muscular organ roughly the size of a closed fist. It sits in the chest, slightly to the left of center. As the heart contracts, it pumps blood around the body. It carries deoxygenated blood to the lungs where it loads up with oxygen and unloads carbon dioxide, a waste product of metabolism.What is the physiology of the heart?
Cardiac physiology or heart function is the study of healthy, unimpaired function of the heart: involving blood flow; myocardium structure; the electrical conduction system of the heart; the cardiac cycle and cardiac output and how these interact and depend on one another.Who is at risk for heart failure?
Coronary artery disease, heart attack, and high blood pressure are the main causes and risk factors of heart failure. Other diseases that damage or weaken the heart muscle or heart valves can also cause heart failure. Heart failure is most common in people over age 65, African-Americans, and women.Can you live 20 years heart failure?
Life expectancy with congestive heart failure varies depending on the severity of the condition, genetics, age, and other factors. According to the Centers for Disease Control and Prevention (CDC), around one-half of all people diagnosed with congestive heart failure will survive beyond five years.What are the signs of worsening heart failure?
Warning signs of worsening heart failure- Sudden weight gain (2–3 pounds in one day or 5 or more pounds in one week)
- Extra swelling in the feet or ankles.
- Swelling or pain in the abdomen.
- Shortness of breath not related to exercise.
- Discomfort or trouble breathing when lying flat.
- Waking up short of breath.

