Does osteomyelitis show on X-ray?
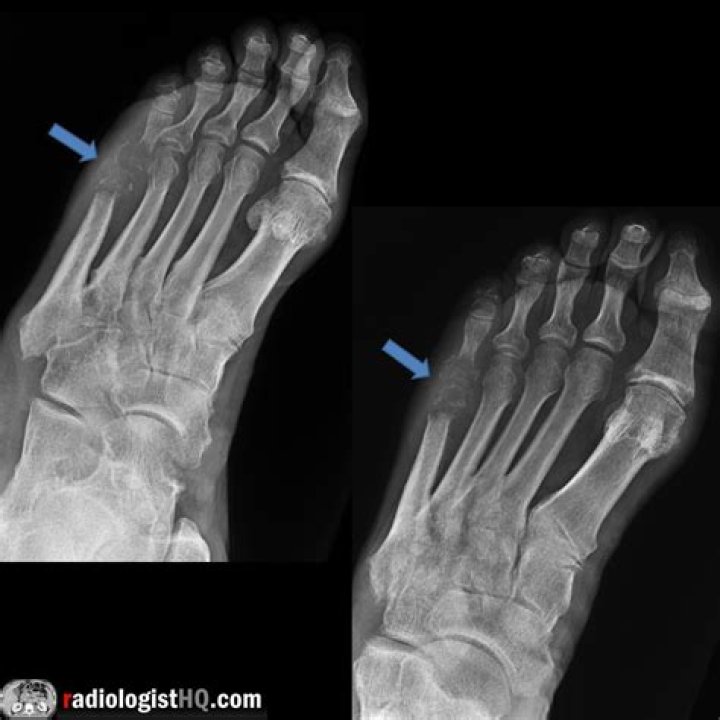
Does osteomyelitis show on X-ray?
Imaging tests X-rays can reveal damage to your bone. However, damage may not be visible until osteomyelitis has been present for several weeks. More-detailed imaging tests may be necessary if your osteomyelitis has developed more recently.
What does osteomyelitis look like on a bone scan?
The features of acute osteomyelitis that may be visible include a periosteal reaction secondary to elevation of the periosteum (Figure 2), a well-circumscribed bony lucency representing an intraosseous abscess (Figure 3) and soft tissue swelling.
Can infection be seen on xray?
Broken Bones and Infections: The most commonly-known use for X-rays. Infections typically cause tissue reactions which are easily visible in an X-ray, and broken bones would be visible to the naked eye if they weren’t covered by skin.
How long does osteomyelitis take to show on xray?
In general, osteomyelitis must extend at least 1 cm and compromise 30 to 50% of bone mineral content to produce noticeable changes in plain radiographs. Early findings may be subtle, and changes may not be obvious until 5 to 7 days in children and 10 to 14 days in adults.
How do you test for osteomyelitis?
How is osteomyelitis diagnosed?
- Blood tests, such as: Complete blood count (CBC).
- Needle aspiration or bone biopsy. A small needle is inserted into the affected area to take a tissue biopsy.
- X-ray.
- Radionuclide bone scans.
- CT scan.
- MRI.
- Ultrasound.
What blood test shows osteomyelitis?
Blood tests: When testing the blood, measurements are taken to confirm an infection: a CBC (complete blood count), which will show if there is an increased white blood cell count; an ESR (erythrocyte sedimentation rate); and/or CRP (C-reactive protein) in the bloodstream, which detects and measures inflammation in the …
How does osteomyelitis look on MRI?
Typical findings of osteomyelitis seen on MRI are decreased T1 signal and increased T2 signal due to marrow edema. However, these can also be seen in the setting of stress reaction, reactive marrow, neuropathic arthropathy, and arthritis.
How do you confirm osteomyelitis?
What test detects osteomyelitis?
The preferred diagnostic criterion for osteomyelitis is a positive bacterial culture from bone biopsy in the setting of bone necrosis. Magnetic resonance imaging is as sensitive as and more specific than bone scintigraphy in the diagnosis of osteomyelitis.
Is WBC elevated in osteomyelitis?
The white blood cell count is often normal even in the setting of acute osteomyelitis. The erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) are often elevated; however, they both lack specificity in the absence of other radiologic and microbiologic data.
Do you need IV contrast for osteomyelitis?
MRI with and without IV contrast is also recommended to evaluate for osteomyelitis and to determine the degree of infection; MRI without IV contrast is appropriate if contrast is contraindicated; CT with IV contrast is appropriate if MRI is contraindicated.